Research

List
Current Projects
Feasibility of Using a Depth Camera or Pressure Mat for Visual Feedback Balance Training with Functional Electrical Stimulation
Individuals with spinal-cord injuries (SCI) are at an increased risk of falling due to their impaired ability to maintain balance. Our research group has developed a visual-feedback balance training (VFBT) system coupled with closed-loop functional electrical stimulation (FES) for rehabilitation of standing balance (FES+VFBT system). As an extension to this system, our lab looked at replacing the force plates used for center of mass (COM) feedback with more accessible, commercial alternatives like a pressure mat or depth camera. Our lab's recent studies showed the depth camera as the better option with performance at least on par with the force plate for providing COM feedback.
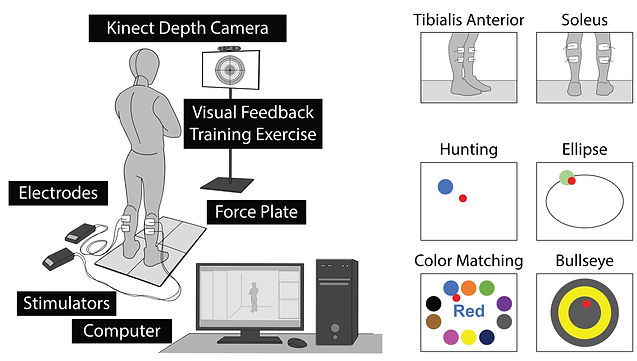
Investigate the Effects of Ankle Muscle Co-Contraction on Ankle Muscle Stiffness and Standing Balance
Spinal cord injury can result in various impairments in the motor system (e.g., increase postural sway during standing). These individuals often utilize co-contractions of ankle joint muscles, simultaneous activation of plantarflexors (e.g., soleus) and dorsiflexors (e.g., tibial anterior). Previous studies showed ankle joint plays a critical role in maintaining balance during standing; and ankle mechanical joint stiffness can be increased as a result of muscle co-contractions. We aim to quantitatively investigate the effects of ankle muscle stiffness on ankle joint stiffness and postural stability and the causal relationship between ankle muscle co-contraction, and postural sway.

Effects of Functional Electrical Stimulation on Facial Muscle Activation and Neurophysiological Responses
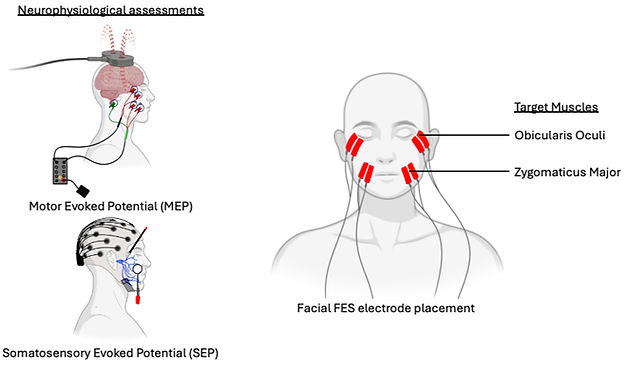
Functional electrical stimulation (FES) has been widely used to restore motor function and enhance neuromuscular control. Our lab is investigating a novel application of FES targeting facial muscles to evaluate its effects on motor and sensory pathways. Specifically, we aim to quantify neurophysiological changes associated with FES-driven facial muscle activation using motor evoked potentials elicited through transcranial magnetic stimulation and sensory evoked potentials recorded via electroencephalography (EEG).
We hypothesize that FES applied to facial muscles modulates corticobulbar excitability and induces neuroplastic changes in sensorimotor networks. To assess these effects, EEG and EMG recordings will be analyzed pre- and post-FES therapy to characterize changes in cortical reactivity and connectivity. By investigating the impact of facial FES on neurophysiological markers, we aim to further our understanding of its potential applications in neuromodulation.
The Neural Circuits in Balance: Investigating Corticomuscular Connectivity in Maintaining Standing Posture
The motor cortex plays a significant role in controlling voluntary movement, by providing descending motor commands directly to effector muscles via transduction along the corticospinal pathway. Conversely, in postural control, particularly during standing balance, muscle activations are dominantly regulated through the reticulospinal and vestibulospinal pathways. However, it is also speculated that modulation of motor commands through the corticospinal pathway is present and critical to the wholistic maintenance of upright balance. We aim to investigate the spectral-temporal evolution of cortical contributions to the control of static and dynamic standing balance.

Mechanism for plasticity in FES therapy
Individuals with motor incomplete spinal cord injury (iSCI) may have some residual ability to stand and walk, but iSCI makes maintaining their balance difficult. Recently, repetitive application of functional electrical stimulation on upper extremities with voluntary efforts, known as functional electrical stimulation therapy (FEST), has been shown to increase the corticospinal excitability resulting in improved motor functions. Although its mechanism of action remains poorly understood, it is hypothesized that repetitive, pairwise neural activations cause long-term potentiation in the motor neural circuit like increasing the bandwidth of an internet connection between a computer and servers. Further, FEST has yet to be utilized on the plantarflexor muscles which are critical to maintaining upright posture.

FES standing balance therapy
Fall risk after incomplete spinal cord injury (iSCI) can be reduced with standing balance rehabilitation. Two noteworthy therapies include visual feedback training (VFT) and functional electrical stimulation (FES). Our lab developed a novel standing balance therapy combining VFT with FES targeting ankle plantar/dorsiflexors. FES amplitude was regulated using PD control with gravity compensation and asymmetric leg biasing to mimic the human physiological controller. Our lab hypothesized that combining these two methods can result in a more effective standing balance rehabilitation therapy for individuals with iSCI. (https://doi.org/10.1186/s12984-021-00861-z, https://doi.org/10.3389/fneur.2020.00680)

Reducing muscle fatigue in functional electrical stimulation for rehabilitation exercises
Spinal cord injuries (SCI) often lead to limited motor capabilities and clinical exercises have been developed with functional electrical stimulation (FES) for individuals with SCI to exercise despite their limited motor capacity. However, current clinical applications of FES exercise is limited by rapid onset muscle fatigue and reduces overall exercise time.
Previous work in our lab have shown that a novel method of delivering stimulation, spatially distributed sequential stimulation (SDSS), is effective at reducing muscle fatigue than traditional single electrode stimulation (SES). But it is unknown whether SDSS is more effective than SES in an exercise setting. As such, we are interested in investigating the fatigue reducing effects of SDSS in FES rowing exercise and the impact on exercise and cardiovascular performance for incomplete SCI individuals. (https://doi.org/10.1016/j.apmr.2021.01.075)

A Novel Combined Neuromodulation Therapy to Enhance Balance and Neuroplasticity after Incomplete Spinal Cord Injury
Improving upright balance is a critical challenge for individuals with incomplete spinal cord injury (SCI). Non-invasive neuromodulation therapies, including transcutaneous spinal cord stimulation (TSS) and functional electrical stimulation (FES), have demonstrated potential in enhancing motor recovery following SCI. This project seeks to evaluate the feasibility and therapeutic effects of a novel neurorehabilitation program that combines TSCS and FES with visual feedback balance training (VFBT) to improve standing balance and promote motor recovery in individuals with incomplete SCI.
Previously developed systems that integrate FES with VFBT have shown promise in enhancing balance by electrically stimulating ankle muscles via a closed-loop system. However, these prototypes have been limited to individuals capable of standing independently. In contrast, TSS has emerged as a promising intervention due to its ability to increase spinal network excitability and facilitate voluntary motor control, especially when combined with active rehabilitation techniques. This project will assess the feasibility of applying TSCS in conjunction with FES during VFBT to individuals with incomplete SCI, aiming to improve balance and stimulate neuroplasticity. By exploring the combined effects of TSCS and FES, the project seeks to provide a deeper understanding of how these technologies can support motor recovery and neuroplasticity in a population with significant rehabilitation needs. The ultimate goal is to expand the application of neurorehabilitation systems to a broader range of individuals, including those who may not be able to stand independently.

Past Projects
Co-contractions may decrease postural stability in individuals with SCI
Individuals with incomplete spinal cord injury (iSCI) often have reduced standing balance ability. It is hypothesized that the muscle activation pattern is affected after spinal cord injury, resulting in reduced balance ability. Specifically, larger co-contraction of the tibialis anterior (TA) and plantarflexor muscles is expected in individuals with iSCI compared to able-bodied individuals. This has previously been shown to be true in the elderly population, but the difference between healthy and individuals with SCI has not been explored (https://doi.org/10.1038/s41598-021-99151-w)

Investigating the Control of Standing Posture
Postural control is a complex task that requires active control of the muscles through both the spinal cord and the brain. We aim to determine the level at which postural control is modulated during standing balance using various measures of excitability and connectivity between the brain, spinal cord, and muscles.

Identification of the postural control system in standing balance
Assessment of standing balance control is important in providing effective therapy and assistive technologies for elderly population and individuals with neurological disorders, such as stroke or spinal cord injury. Parametric system identification has been used to quantitatively assess one’s postural control system. However, such technique is not clinically feasible as it requires laboratory-grade equipment. Our lab proposed novel system identification method that is clinically-feasible but has not been compared with conventional system identification method. Here, we aim to compare the accuracy of our system identification method.

Reactive balance in response to simulated forward fall in individuals with incomplete spinal cord injury
Individuals with incomplete spinal cord injury experience impairment of the lower-limb sensorimotor functions. These individuals often show compromised reactive standing balance and are faced with increased risk of falls. We investigated how the foot placement was affected in individuals with incomplete spinal cord injury during simulated forward falls.

Ankle-hip joint coordination play important role in regulating postural sway
While ankle joint acts as the first respondent in regulating postural sway during quiet standing. Many highlighted the importance of the hip joint as well as the coordinated activity between the two joint dynamics. Specifically, the anti-phase relationship between the ankle and hip joint acceleration make significant contribution towards reducing the center-of-mass acceleration. We investigated how this inter-joint coordination is affected in individuals with incomplete spinal cord injury and how the inter-joint coordination is related to the overall postural sway (https://doi.org/10.1152/jn.00302.2020).

Brain muscle networks in individuals with incomplete spinal cord injury
Individual with incomplete SCI (iSCI) exhibit gait and posture disorders due to defective communication between the brain and muscles. To reveal the effect of SCI on the cortical control of muscles during standing and walking, we investigate the differences in the brain-muscle connectivity (i.e., how brain communicates to muscles) between iSCI patients and healthy people during walking and standing, and 2) relationships between residual motor functions and the brain-muscle connectivity in individuals with iSCI.

Cosine tuning determines plantarflexors’ activities during human upright standing
Human bipedal stance is inherently unstable. Plantarflexors including the soleus (SOL) and medial gastrocnemius (MG) play key roles in controlling the bipedal stance; however, how the central nervous system controls the activation levels of these plantar flexors is not well understood. It is known that the brain modifies the muscle activation level in a cosine tuning manner where the maximal activation is achieved in a preferred direction (PD) for each muscle. We are interested in investigating whether plantarflexors’ activations follow a cosine tuning manner during bipedal quiet standing. Additionally, how spinal cord injury detrimentally affects standing balance, which may be due to impaired neural control of plantarflexors. (https://doi.org/10.1152/jn.00123.2020)

Spinal paired associative stimulation using motor point stimulation
Individuals with incomplete spinal cord injury (iSCI) may suffer from life-long motor impairments from a severed connection between the brain and muscles below the level of injury. Recent studies have shown that repetitive carefully timed stimuli (I.e. spike timing dependent plasticity) colliding at the spinal cord can improve the efficacy of the remaining connections and improve motor function. Due to the novelty of this type of intervention, many challenges are left to be addressed. Among these challenges, we are interested in determining a method of applying this intervention to any muscle affected by iSCI and investigating further the mechanism of STDP and its applicability for iSCI interventions. (https://doi.org/10.3389/fnhum.2020.593806)

Effect of FES on the reactive balance in individuals with incomplete spinal cord injury
Our lab has previously explored the effect of perturbation-based balance training (PBT) on improving the reactive balance of individuals with incomplete spinal cord injury (iSCI). We are now investigating the potential effect of augmenting PBT with functional electrical stimulation (FES). We believe that this novel intervention, termed PBT+FES, will improve the reactive balance in the iSCI population. The reactive balance in participants will be measured using the lean-and-release technique, where the resulting foot placement will be analyzed using the concept of margin of stability (MOS). By improving reactive balance, we aim to reduce falls in the iSCI population.

